Originally published in Planetalk
In the multi-priority world of hospital administration, it is a rare and precious occurrence when “the right thing to do” coincides with business opportunity. However, an established and still-growing body of data, both hard and anecdotal, indicates that a patient-centered approach to the planning and design of hospitals, medical clinics and outpatient facilities, and retirement villages and continuing care facilities is the rare case where “too-good-to-be-true” is simply a fact. The implications are broad-ranging. Industry experts now agree that the physical environment where care is received, in conjunction with other patient-centered care principles, provides enormous opportunity for improving the quality of patients’ health care experience and actually accelerating the healing process. It is not simply that patients fare better in an environment that provides for their social, cultural, and intellectual needs–it is that hospitals that create environments conducive to fulfillment of these needs can expect to see significant improvements in patient satisfaction, positive patient outcomes, and employee engagement that ultimately save money.

Together with Planetree, HMC Architects has co-authored a paper, Design and the Bottom Line: Practical Patient-Centered Approaches to the Physical Environment, that discusses misconceptions about the long- and short-term costs associated with the evolution of a hospital or campus toward a patient-centered design, as well as the prevalent tendency to dismiss changes to the physical care-delivery environment as insubstantial or irrelevant to the organization’s bottom line. The perfect storm of more satisfied patients, better outcomes, less costly care, and staff who never want to leave can be achieved by incremental changes over time, as an integral part of a hospital’s capital improvement, renovation, or expansion budget.
The paper explores four primary categories that comprise the business case for investing in the design of patient-centered care environments:
1. Outcomes that are produced in the hospital: the success rate of individual procedures, including the need for follow-up care, and reduction in the length of average stays. (The latter is a source of substantial savings.)
2. Attracting users: creating an inviting and navigable setting for both patients and their families, and for staff that provides varied areas for privacy, interaction, family time, contemplation, and contact with the outdoors.
3. Human resources impact on the bottom line: the number of productive hours per patient day at all staff levels, impact on staff retention, and effect on recruitment.
4. Repeat business: Reputation in the community; continued patient and family patronization, especially in choice-driven scenarios such as obstetrics and pediatrics; the ability to attract new patients and garner additional donations.
While it is possible and, in many project instances, desirable to make incremental changes to the physical environs of a hospital once leadership has realized the value, imparting therapeutic or “healing value” goes beyond changing a few paint colors or light bulbs. It requires a thorough understanding of the needs and expectations of patients and staff, the purpose and practices of the health care facility, and the psychological and social effects of design and planning. Because the cultural identity, type of illness, lengths of stay and physical/psychological constraints may vary substantially from one patient to the next, a successful patient-centered design must strive to foster a full spectrum of positive and uplifting psychological responses, including:
Privacy and undisturbed rest/contemplation.
Creating an inclusive environment that welcomes families and allows them to be involved in care.
Mobility and exploration of communal areas.
Separation between staff and patient areas, allowing staff to “go offstage.”
Ownership/control of immediate surroundings.
Socialization and interaction with others.
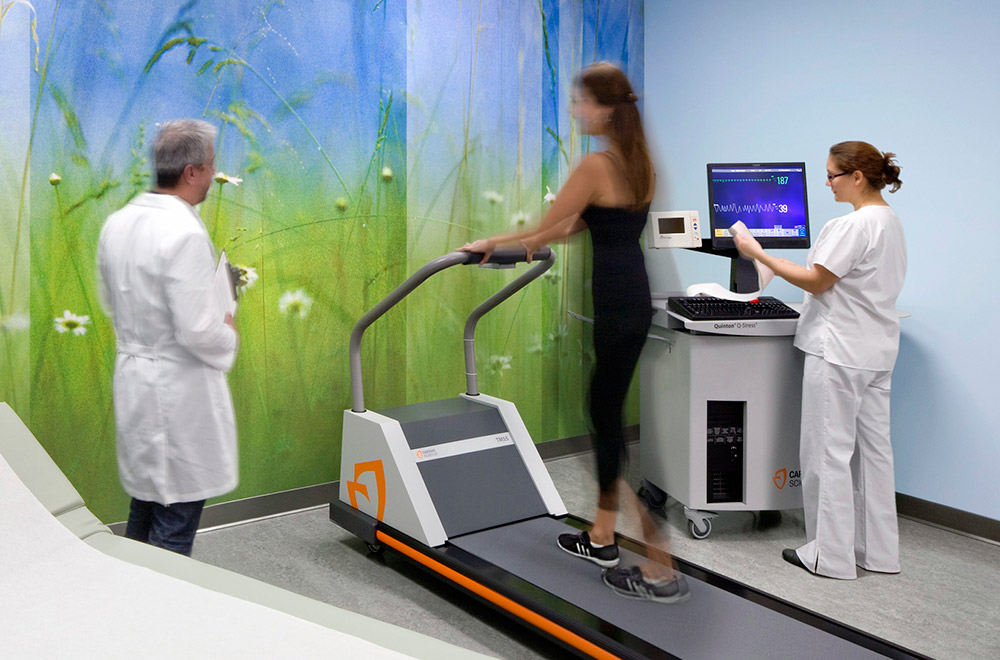
“Bringing the outside in:” integrating patients with nature via views, artwork, landscape, and water features.
Creating opportunities for patients to be outdoors where feasible.
Some hospitals tackle the transformation in a concentrated way; some do it over years to defray costs. There can be a plan for every budget that will empower patients and family members as part of the healing process, enrich the surrounding community, and save money in the long term. Learn more by downloading the entire white paper, follow the 10-part blog series, and use the #planetree hashtag to contribute to the conversation on Twitter.