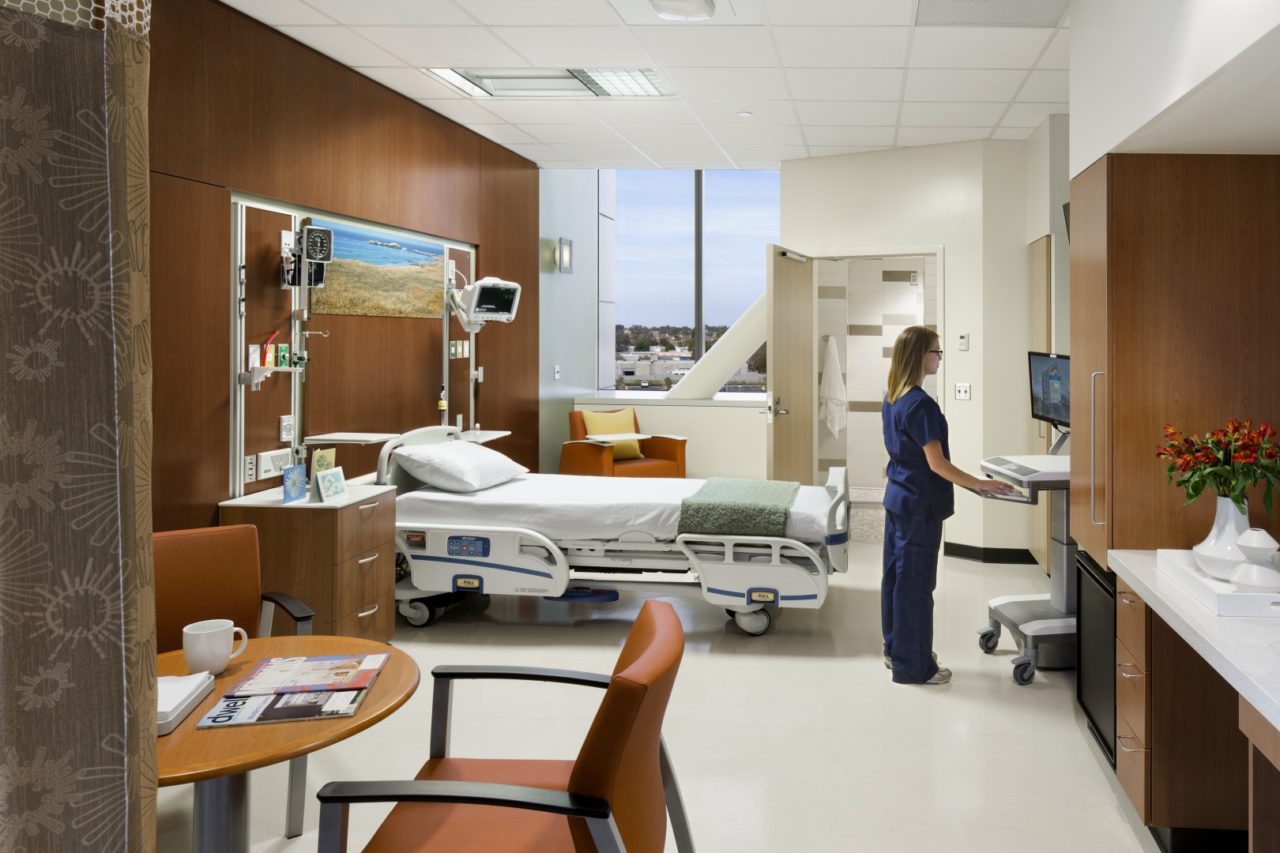
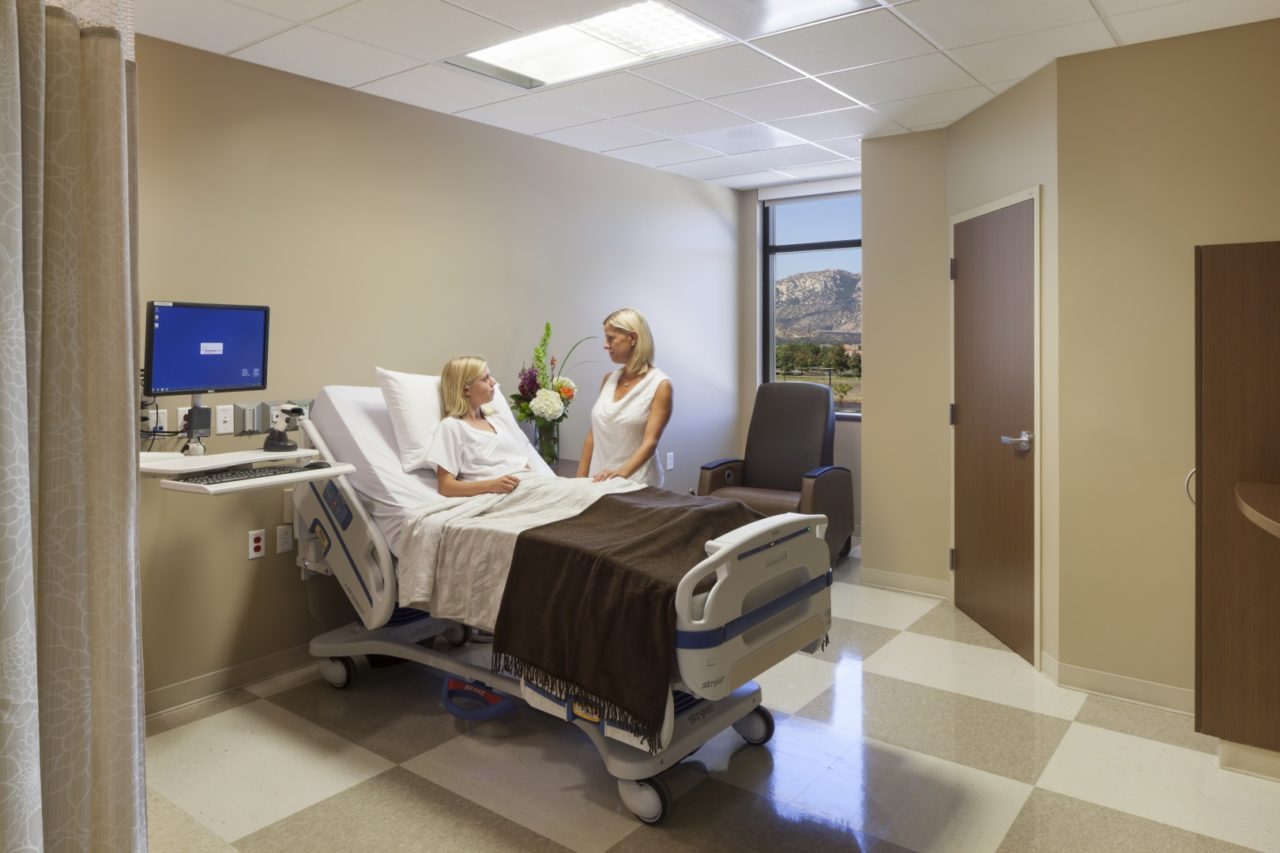
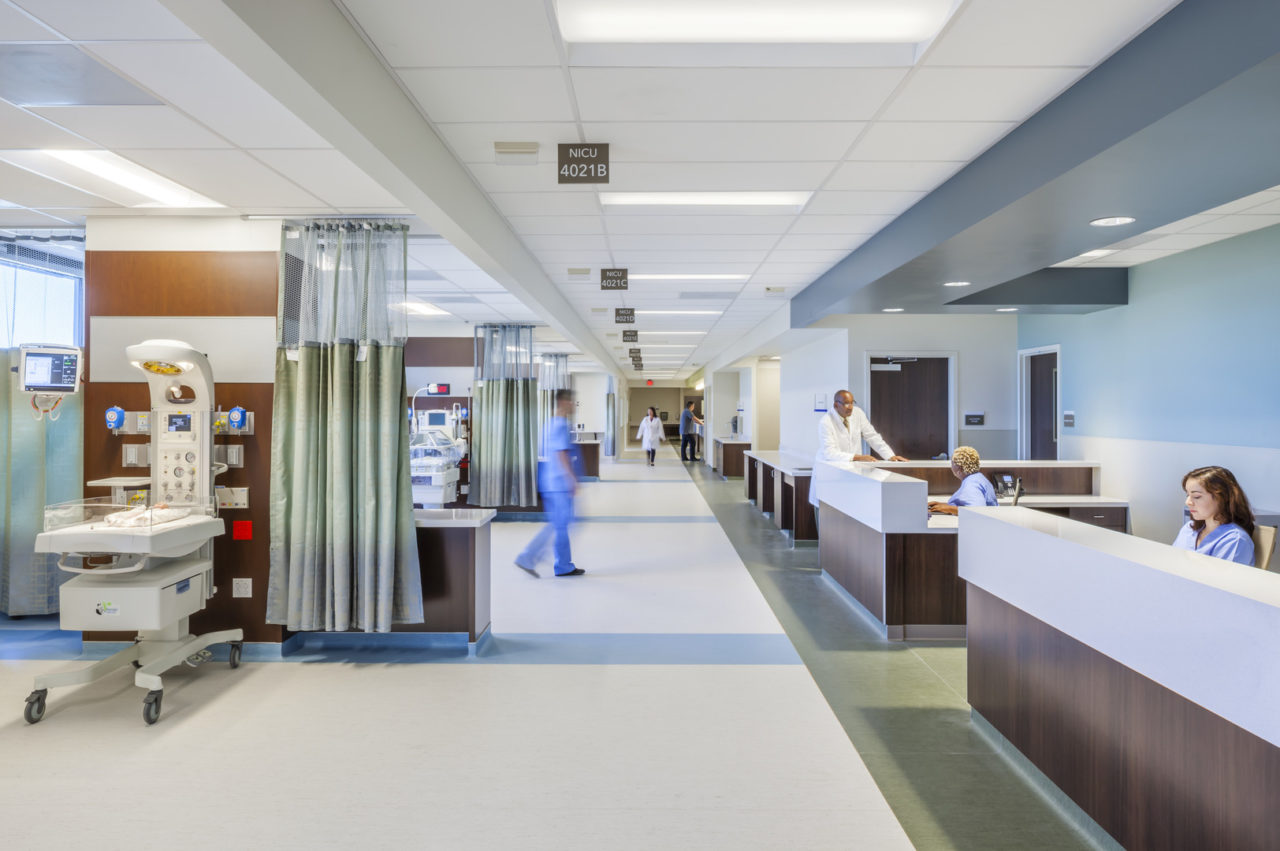
Patients and staff both rely on both privacy and confidentiality to ensure a safe, professional time in a healthcare space. Designing for privacy is one way healthcare architects aid in legally protecting patient records, prescriptions, and examinations from being shared or accessed by anyone other than his or her case physician. Designing for confidentiality, however, protects the actual information disclosed by a patient to a caregiver during dialogue in a medical visit. Privacy and confidentiality are related, but are two individual concepts. The biggest difference between the two is the role of law, however, ethics are fundamental with confidentiality. In an upcoming post, we will discuss in more detail how confidentiality works in healthcare design. Today, our primary concern is architecture and privacy; in other words, how a healthcare space can be designed for privacy.
The Challenges of Designing for Privacy
Respect for patient privacy and assuring patient confidentiality have been regarded as essential obligations of healthcare providers and primary responsibilities of healthcare institutions under the New Health Insurance Portability and Accountability Act (HIPAA). As a result, HIPAA has spurred on a greater awareness of–and sensitivity to–patient privacy across multiple spectrums in hospital settings. Many of these standards and regulations will be satisfied with some minimum requirements; however, sticking to those minimums has become obsolete for 21st-century medical practices. As patients and their families have more choices in the marketplace, the amenities provided become more important. And, since it’s been proven that privacy has one of the greatest impacts on patient care delivery, patient well-being, and, of course, the cost of operation and revenue, many healthcare organizations are striving to create better spaces built to higher standards based on best practices to achieve greater provider/patient satisfaction.
Why Is Architectural Privacy Important to Healthcare?
Privacy and confidentiality, in the context of healthcare design, are both imperative for several reasons and the value of promoting trust in healthcare environments by implementing privacy factors is of great importance for both patients and health providers. Building trust between the patient and healer or the patient and a healing environment are essential for healing itself to occur. Privacy in healthcare facility settings is widely recognized as a necessity in the development of trustworthy, ethical environments.
Privacy is closely linked with trust. Patients are vulnerable emotionally, physically, spiritually, and often financially.
When patients feel like their privacy is valued, they can begin to trust their provider. Once patients and caregivers build trust, the trustworthiness of their environment becomes essential to the patient’s overall well-being. If a patient has difficulty developing trust in their healthcare providers–perhaps because they aren’t being given enough privacy–efficient use of both the patient’s and the physician’s time will be greatly impacted in a negative way.
The ethical environment in a healthcare organization has a positive effect on healthcare providers as well. A trustworthy working climate has positive effects on job satisfaction, employee retention, ability to manage conflict, and patient outcome. A lack of the privacy needed by caregivers to discuss medical information with their patient or other medical staff will create operational inefficiencies and have a negative impact on the patient’s perception. The leaders of healthcare architecture organizations play a key role in designing, building, maintaining, and encouraging an ethical environment and climate. It is one of the main responsibilities of design leadership to create elements of privacy in an ethical healthcare environment not only to initiate and maintain trust between patients, caregivers, and their healthcare environment, but also encourage good practice.
This concept of privacy doesn’t solely affect the patient, either; federal regulations and requirements mandate certain levels of privacy for care providers and staff. Patient friends and family members are also impacted by the availability of privacy. For these reasons, the standard of care has shifted to provide more privacy in design and elements that showcase trust. Private rooms increase patient and family satisfaction–in competitive markets, this is a key advantage. Privacy also has various implications for different types of healthcare facilities, in particular inpatient, outpatient, and emergency services.

Architectural Privacy and Patient Visibility
In many ways, designing for privacy is a very physical concept. Architectural privacy refers to the visual and acoustic isolation supplied by an environment. Are spaces designed to present information access? Can sessions and appointments be conducted without the risk of someone overhearing sensitive medical details? If a practice answers “no” to any of these questions, there may be some fundamental privacy design errors on display.
Visual privacy can also serve as a function of the spatial arrangements of spaces. Often, we tend to view privacy and visibility as similar in healthcare when they actually serve different functions. Patient acuity determines the importance of visibility versus privacy for patients. The higher the level of acuity, the more the patient needs observation by clinicians. In healthcare spaces with lower staffing levels, it’s important that the practice not be too spread out. Instead, the space needs to be easily navigated so patients can be properly attended to without compromising their privacy in any way.
In less acute settings, both acoustic and visual privacy for both patients and family become primary. Since the patients and family might not need heightened levels of clinician attendance, it’s important to give them a private space, whether for waiting or treatment. There are numerous ways to bring architecture and privacy together in a health facility; however, the type of facility and level of patient acuity are important factors in determining what techniques will be most effective
New Techniques for Improving Patient Privacy
In the twentieth century, taking advantage of technological advances is critical. A lot of new facilities are moving toward deploying privacy-enhancing technologies.
Self-rooming technology: Using this technology, patients can check in at a kiosk at the front of the clinic and receive a badge connected to an electronic monitoring service. They are monitored electronically and physicians can locate and direct them to an exam room. All patient data is transferred to caregivers’ computers, allowing care teams to manage patient flow effectively and without the interaction of patients with anyone prior to situating in their private exam or consultation rooms along with their trusted family members.
Online check-in: In new facilities (mostly urgent care or emergency services), patients can check in online using their mobile device, choose the location they will visit based on wait times or proximity, start populating their information to the chosen facility, and begin to interact electronically via text messaging. This technique minimizes the need for registration work and respects the privacy of patients by skipping the step of providing their private information in a public environment.
Telehealth or remote home healthcare: Due to the rapid pace of innovation, voluntary codes can help provide guidance on some situations and new technologies; however, physicians will need to stay informed of their institutions’ privacy and security policies and discuss these with patients as part of their ethical obligation to ensure patient-physician confidentiality. Also, the quality of the environment that caregivers use to communicate with their patients via the internet plays a large role to gain that trust. A high-quality environment incorporates enclosed private spaces with full control of sound disturbance.

HMC Architects on Designing for Privacy
At HMC Architects, we value patient, staff, and family privacy in all healthcare spaces. Starting from the root in our design process, we use an integrated, collaborative process that focuses on the design, construction, operation, and occupancy of a building over its complete lifecycle. This allows the design team to meet and interview caregivers and some patient-family committees during the design phase and collect data, concerns, and feedback in order to establish the right goal for the project, set the bar higher, and, ultimately, design a trustworthy space that improves patient and caregiver flow and experience. One of the main elements of integrated design is trust between design team members, the client, and end users. At HMC Architects, we ensure this trust is reflected in all our design aspects.
As such, we design medical facilities to be representative of that belief. At Henderson Hospital in the Las Vegas area, we prioritized patient satisfaction as a marker of success. This meant privatizing rooms and reducing noise. The patient area was developed to be calming and quiet thanks, in part, to the isolation of the nurse’s station behind glass walls and a silent nurse call function that operated via a wireless system.
At the Torrance Memorial Medical Center Lundquist Tower, we created private rooms that provided ample space for patients, guests, and staff. By modernizing these rooms and prioritizing the patient’s satisfaction as a guest in the facility, we put the focus back on healing and well-being.
Innovation continues and our design solutions are evolving. Our design team conducts constant assessments to ensure goals are met and to develop tailored solutions that yield additional value while meeting requirements and goals.
Some of the solutions we employ in our design are:
- Private, instead of semi-private, in-patient rooms
- Enclosed patient emergency bays instead of curtain separation
- Operable integrated blinds in windows
- Cubicle curtains
- Zoning patient rooms for activities: provider, patient, and family members
- Separation of the path of travel for patient movement versus the public (gowned patients in gurneys)
- Zoning of waiting areas for different activities including private work, TV watching, and kids’ activities
- Acoustic separation of spaces
- White noise